Why You’re Constipated in Perimenopause (And What to Do About It)
Foods and supplements to increase your fiber intake, and finally get things moving again.
Let’s talk about something nobody puts on their perimenopause symptom bingo card, but absolutely should.
Constipation. Sluggish digestion. That uncomfortable, bloated, nothing-is-moving feeling.
If this sounds familiar, I want you to know: you are not imagining it, and you are definitely not alone.
When I ask women in perimenopause what their biggest frustrations are, hot flashes and sleep usually top the list. But somewhere in the middle — often said with a slightly embarrassed laugh — comes the digestive stuff.
The bloating. The irregularity. The days when it feels like your gut has simply… stopped cooperating.
The truth is, constipation is one of the most common — and most under-discussed — symptoms of perimenopause. And there’s very real science behind why it happens. More importantly, there’s a lot you can do about it through food and targeted supplements.
Let’s dig in. 🌿
“Your gut is not broken. It’s responding to a dramatic hormonal shift — and it needs your help to adapt.”
Why Perimenopause Messes With Your Digestion
During perimenopause, estrogen and progesterone levels don’t just decline — they fluctuate wildly before eventually dropping for good. This hormonal rollercoaster has a direct impact on your gastrointestinal tract in several ways.
Estrogen and gut motility: Estrogen plays an important role in regulating the speed at which food moves through your intestines (a process called gut motility). As estrogen fluctuates and declines, your intestinal muscles can become slower and less coordinated — meaning food takes longer to move through, and constipation sets in.
Progesterone and smooth muscle relaxation: While progesterone has a muscle-relaxing effect throughout the body (which is why it can cause constipation during the luteal phase of your cycle), its instability in perimenopause disrupts the normal rhythm your digestive system has relied on for decades.
Your gut microbiome changes too: Research is increasingly showing that the gut microbiome — the community of trillions of bacteria living in your intestines — changes significantly during perimenopause. A less diverse microbiome can directly contribute to slower transit time, bloating, and difficulty passing stools.
Cortisol and stress: Perimenopause is often accompanied by disrupted sleep and elevated stress, and chronically high cortisol signals your gut to slow down. The gut-brain axis is incredibly sensitive, and your nervous system running on empty doesn’t help things move along.
Signs your constipation may be hormone-related:
It’s gotten notably worse in your 40s or early 50s despite no major diet changes
You notice it fluctuates with your cycle (or what’s left of it)
It comes paired with bloating, gas, and that “full but nothing moving” feeling
You’re also experiencing other perimenopausal symptoms like brain fog, poor sleep, or hot flashes
It coincides with increased stress or periods of poor sleep
Fiber: Your First Line of Defense
If there is one non-negotiable nutritional intervention for perimenopausal constipation, it’s fiber. Full stop. And yet, most women are getting nowhere near enough of it.
The recommended intake for women over 50 is 21–25g of fiber per day, but research consistently shows that most women are consuming closer to 12–15g. And for those navigating the hormonal shifts of perimenopause? I’d actually argue that aiming for 30g or more is the sweet spot for optimal gut health and hormone support.
Here’s why fiber is so powerful in perimenopause specifically:
First, fiber adds bulk and moisture to your stool, making it easier to pass.
Second — and this is the part that doesn’t get talked about enough — fiber helps your body metabolize and eliminate used estrogen.
When you eat enough fiber, your liver’s detoxified estrogen gets bound up in the gut and excreted. When you’re low on fiber, that estrogen can be reabsorbed, contributing to a hormonal imbalance.
Eating fiber isn’t just about your gut — it’s literally supporting your hormone health.
Third, fiber is the primary food source for your gut bacteria. A fiber-rich diet actively nourishes a diverse, thriving microbiome — which, as we’ve seen, is especially important during this life stage.
The two types of fiber — and why you need both
Soluble fiber dissolves in water to form a gel-like substance in your gut. It slows digestion in a helpful way, feeds beneficial bacteria, and helps soften stool. Think: oats, flaxseeds, apples, legumes.
Insoluble fiber doesn’t dissolve — it adds bulk and helps move food through your intestines more efficiently. Think: whole grains, bran, leafy vegetables, seeds.
The best approach is to eat a wide variety of both, which is exactly why a diverse, plant-rich diet is so effective. Aim to “eat the rainbow” across the week, including as many different plant foods as possible.
The Best High-Fiber Foods for Perimenopause
Legumes: Lentils (cooked) — 15g/cup | Chickpeas — 12g/cup | Black beans — 15g/cup | Edamame — 8g/cup | Split peas — 16g/cup
Whole Grains: Rolled oats — 4g/cup | Barley — 6g/cup | Quinoa — 5g/cup | Whole wheat bread — 3g/slice | Brown rice — 3.5g/cup
Fruits: Avocado — 10g each | Raspberries — 8g/cup | Pears (with skin) — 5.5g each | Apples (with skin) — 4.5g each | Figs (dried) — 14g/half cup
Vegetables: Artichoke — 10g each | Broccoli — 5g/cup | Sweet potato — 4g medium | Carrots — 3.5g/cup | Brussels sprouts — 4g/cup
Seeds: Chia seeds — 10g/2 tbsp | Ground flaxseed — 4g/2 tbsp | Hemp seeds — 1.2g/3 tbsp | Psyllium husk — 7g/tbsp | Pumpkin seeds — 2g/oz
Nuts: Almonds — 3.5g/oz | Pistachios — 3g/oz | Walnuts — 2g/oz | Almond butter — 3g/2 tbsp | Cashews — 1g/oz
A practical tip: start slowly and increase gradually. If you go from 12g to 35g of fiber overnight, your gut will revolt with gas and bloating.
Add one or two new fiber-rich foods per week, always pairing them with increased water intake — fiber needs water to do its job properly.
Don’t Forget Probiotics and Prebiotics
Fiber is the foundation, but if we want to talk about a truly comprehensive approach to perimenopausal gut health, we need to talk about the microbiome — and the two types of foods that support it most directly: probiotics and prebiotics.
Think of it this way: prebiotics are the food, and probiotics are the workers. You need both for a thriving gut ecosystem.
Prebiotic foods (feeding your good bacteria)
Prebiotics are specific types of fiber that selectively feed the beneficial bacteria in your gut. They’re particularly concentrated in:
Garlic and onions (incredibly potent prebiotics)
Leeks and asparagus (rich in inulin)
Jerusalem artichokes (one of the highest prebiotic sources)
Unripe bananas (high in resistant starch)
Chicory root (the original inulin source)
Cooked and cooled potatoes or rice (resistant starch)
Oats and barley (beta-glucan)
Probiotic foods (introducing beneficial bacteria)
Probiotic foods contain live cultures of beneficial bacteria that, when consumed regularly, help populate and diversify your gut microbiome. Research suggests that a more diverse microbiome is associated with better hormonal regulation, improved mood, stronger immunity, and — yes — more regular bowel movements.
Plain, full-fat yoghurt with live cultures (look for “live active cultures” on the label)
Kefir — one of the most powerful probiotic foods available
Sauerkraut — raw, unpasteurized is key (not the one made with vinegar)
Kimchi — fermented cabbage, also rich in prebiotics
Miso paste — fantastic in soups and dressings
Tempeh — fermented soy, also a great protein source
Kombucha — choose lower sugar versions
Aged cheeses like Parmigiano Reggiano, Gouda, aged cheddar, and gruyère
A practical goal: try to include at least one probiotic food and one prebiotic food every single day. It doesn’t need to be elaborate — a spoonful of sauerkraut alongside your lunch, some yoghurt with berries, or garlic and onion in your cooking all count.
As a side note, I’ve started making my own sauerkraut, and it’s easier than I thought. If you want to know more, send me an email or leave a comment.
✨ Get Your Gut Health Bundle 🦠🌱
I’ve created this resource specifically for my perimenopause clients, to make it easy to fight against the symptom of constipation.
It includes:
34 probiotic and prebiotic foods clearly organized for fast reference.
48 fiber-rich foods from fruits, veg, legumes, grains & seeds — with fiber content and calorie count per serving so there's no guesswork.
5 delicious gut-health recipes
A complete gut health tracking bundle — daily journal, weekly checklist, and expert tips.
A monthly fiber tracker.
Beautifully designed PDF, available in US Letter, A4 & A5 formats.
Instant download.
Get it now with a 25% discount using the code SUB25
→ Grab Your Copy On My Etsy Shop
Supplements That Can Help
Whole food sources of fiber should always come first — you get so much more alongside the fiber (vitamins, minerals, antioxidants, phytoestrogens). But supplements can be a genuinely useful addition, especially during periods when diet alone isn’t cutting it, or you’re traveling, and routine goes out the window.
Psyllium Husk — A soluble fiber that absorbs water and forms a gel, softening stool and improving transit time. One of the most evidence-backed options for constipation. Start with 1 teaspoon daily and keep adding if needed. I add it to my morning oats with yogurt. Drink plenty of water!
Magnesium Citrate or Oxide — Draws water into the bowel to soften stool. Also helps with sleep, anxiety, and muscle tension — common perimenopausal complaints. Citrate is gentler; oxidate is more laxative. 200–400mg a day is a common starting point. Start low.
Ground Flaxseed — Rich in both soluble and insoluble fiber, plus lignans (plant compounds that act as phytoestrogens — particularly helpful in perimenopause). Add to smoothies, oatmeal, or yoghurt. Use 1–2 tbsp daily; must be ground to absorb properly. Store in the freezer to keep their freshness.
Probiotics (supplement form) — Can help replenish microbiome diversity when diet alone isn’t sufficient. Look for multi-strain formulas with Lactobacillus and Bifidobacterium strains for constipation. CFU count matters less than strain specificity. Take consistently for 4–8 weeks.
Inulin / FOS — A prebiotic fiber supplement derived from chicory root. Specifically feeds Bifidobacterium species associated with regular bowel movements. Start at 2–3g/day and increase slowly to avoid gas.
Aloe Vera Juice — Has a mild laxative effect and may soothe gut inflammation. Choose decolorized, purified forms. 30–60ml before meals. Not for long-term daily use.
Important: Always talk to your healthcare provider before starting new supplements, especially if you’re on medication or managing any health conditions.
The Non-Negotiables Beyond Food
Hydration, hydration, hydration. Fiber without water is like a sponge without liquid. Aim for at least 2-2.5 liters of water per day, more if you exercise. Teas count too, but not coffee! Your morning glass of water is a wonderful gut-activating ritual.
Move your body daily. Physical activity literally moves your bowels. Even a 20–30 minute walk each day can significantly improve transit time. No gym required.
Don’t ignore the urge. When your body signals that it’s time to go, listen to it. Regularly suppressing the urge weakens the reflex over time and worsens constipation.
Establish a morning routine. Your colon is most active in the morning (gastrocolic reflex). Eating breakfast, moving a little, and allowing time to use the bathroom can work wonders.
Try a footstool. Elevating your feet slightly while on the toilet (a squatty potty or even a stack of books) straightens the anorectal angle and makes elimination easier. Sounds silly; works brilliantly.
Manage stress actively. Your nervous system runs your gut. Chronic stress = chronic constipation. Breathwork, gentle yoga, meditation, time in nature — whatever works for you, prioritize it.
🌿 What I Eat Daily To Take Care Of My Gut Health
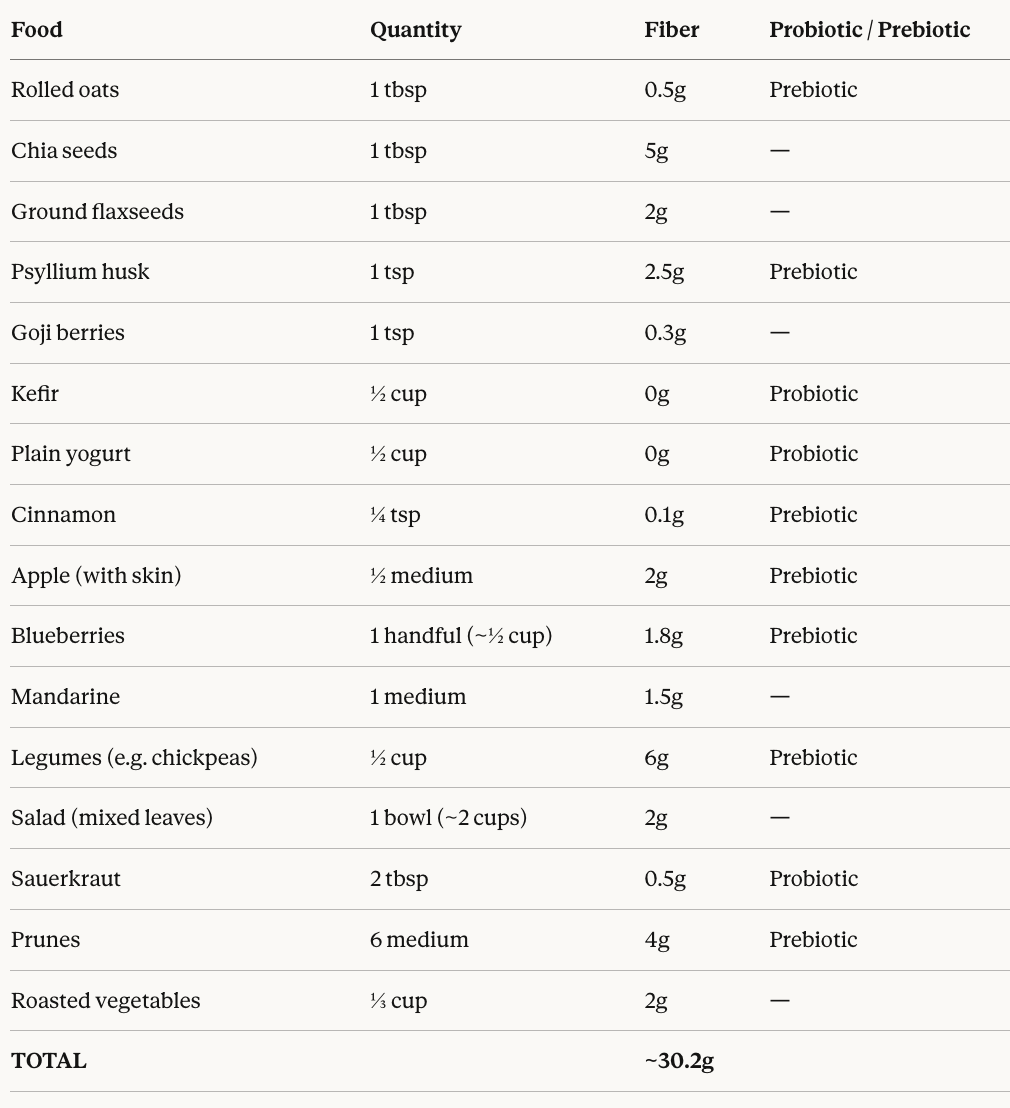
One of the questions I get asked most often is: What does a high-fiber day actually look like in real life? Not a perfect textbook example — but a real, doable, everyday routine. Here’s exactly what I eat most days, and how it all adds up:
That’s 30g of fiber from simple, everyday foods — no complicated recipes, no expensive superfoods, and no forcing it. Just consistent, intentional choices spread throughout the day.
Of course, things might look different some days — if, for example, I add another piece of fruit, and if that fruit is a pear, I easily add 6 more grams. Or maybe one day I skip the salad and have some lentils instead.
When it comes to food, things are constantly changing, but what’s important is to have the right foundation from staple ingredients you eat daily.
The beauty of this approach is that none of it feels like a “health food diet.” Small additions, stacked consistently, that add up to a genuinely well-nourished gut — every single day.
A few things worth noting here. The kefir and yogurt bring zero fiber, but they’re pulling serious weight as probiotics — introducing beneficial live bacteria to the gut.
The sauerkraut does double duty as a probiotic, too, so I never skip it. Meanwhile, foods like the oats, psyllium husk, apple, blueberries, legumes, prunes, and cinnamon are all working as prebiotics — feeding and nourishing the good bacteria already living in your gut.
Of the 16 foods on this list, 3 are probiotics (kefir, yogurt, sauerkraut) and 7 are prebiotics (oats, psyllium husk, apple, blueberries, legumes, prunes, cinnamon) — meaning more than half of my daily eating is actively supporting my gut microbiome, not just hitting a fiber number.
💌 A Final Word
Perimenopause asks a lot of your body. And your gut — quietly, unglamorously — is often one of the first places that starts to struggle. The good news is that this is one area where the right food and lifestyle choices can make a genuinely significant difference, often within just a few weeks.
You don’t need to overhaul everything overnight. Start with one change: add chia seeds to your morning smoothie, swap white rice for lentils a couple of times a week, or have a small serving of sauerkraut with dinner. These small shifts compound into meaningful results.
Your gut is not broken. It’s asking for more support than it needed before. Give it that support, and it will reward you with better digestion, better energy, more balanced hormones, and that elusive feeling of things simply working the way they should.
You’ve got this. 💚
Enjoyed this article? Share it with a friend who might be going through the same thing. The more we talk openly about perimenopause — even the less glamorous parts — the better supported we all feel. 💩✨



This is very insightful. I tried taking two different kinds of fiber supplements but they both caused bloating, gas and constipation. I hear people living fiber supplements and I wish they worked for me as well.